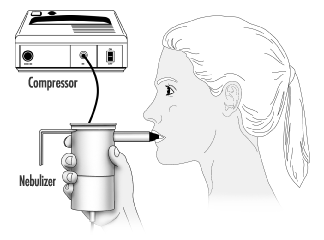
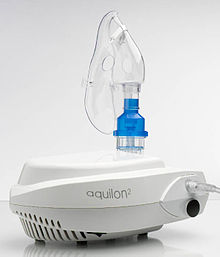
Nebulizer
This study examined the relationship between adherence to domiciliary
nebulized therapy and psychological factors; patient attitudes, anxiety,
depression, and quality of life. Ninety three patients aged 45-77 yrs
with chronic obstructive pulmonary disease (COPD) and using domiciliary
nebulizers were recruited from a hospital database. They completed the
St George's respiratory questionnaire (SGRQ)-1 and the hospital anxiety
and depression scale (HADS) and attended a semistructured interview.
Their usual nebulizers were replaced by Dataloggers, which record the
date, time and duration of each treatment, to use for 4 weeks. The SGRQ
was then repeated (SGRQ-2). Eighty two patients completed the study.
Fifty six percent were poorly adherent; taking less than 70% of the dose
prescribed (or less than 60% on regimens of > or = 5 times daily).
The total scores on the SGRQ-2 were negatively correlated with
percentage adherence. Multiple regression analysis showed that the
SGRQ-2 total score was associated with percentage adherence, depression
score, feeling supported by clinic staff, and patients feeling that they
tried to ignore their chest disease. Patients who report poor quality
of life are more likely to be depressed, feel unsupported by clinic
staff and be poorly adherent to treatment. Increased levels of clinic
support, with the addition of psychological treatments, may be of
benefit to some patients with chronic obstructive pulmonary disease.






No comments:
Post a Comment